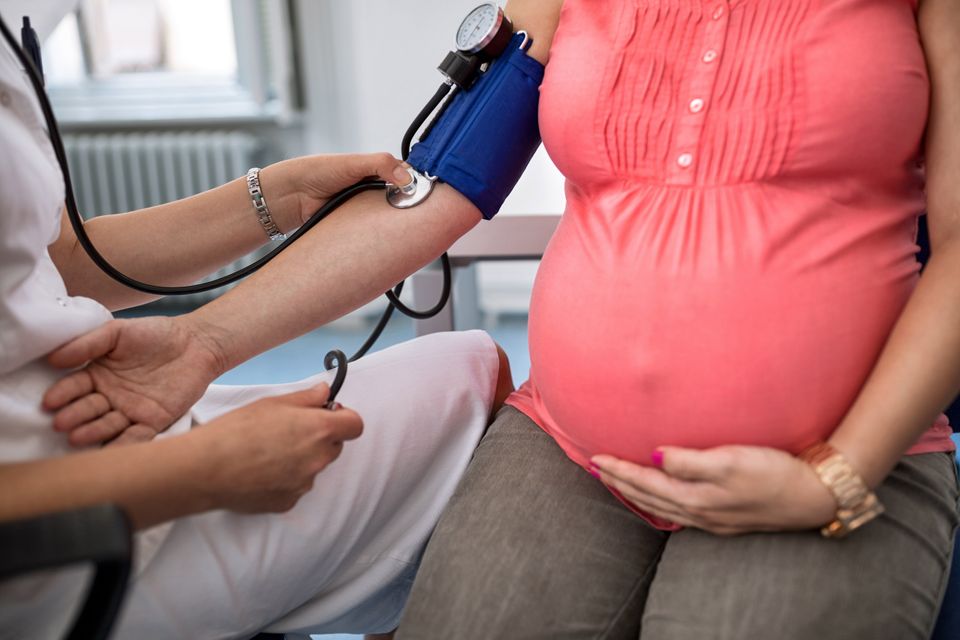
Smoking is the most common preventable risk factor for complications in pregnancy. Quitting smoking can reduce the risk of adverse outcomes for women and their babies. Women are more likely to quit smoking during pregnancy than at any other time of life. Maternity care professionals are well-placed to deliver smoking cessation care to women and their partners.
Quit's 3-step brief advice model Ask, Advise, Help (AAH) is an approach that promotes cessation and aims to connect people who smoke with best practice care.
- Ask all women about smoking status and document this in their medical record. This can include carbon monoxide monitoring, if available.
- Advise all women who smoke to quit and stay quit in a clear, non-judgemental and personalised way, and advise of the best way to quit.
- Help women who smoke to quit by offering a referral to behavioural intervention (for example, Quitline) and consider nicotine replacement therapy (NRT), if clinically appropriate.
Assessment of a woman's motivation to quit smoking is not required and brief advice should be offered at every clinically appropriate opportunity.
Video examples of conversations with patients.
Multi-session behavioural interventions (for example, Quitline) are recommended as first-line therapy in pregnancy.
Quitline is a confidential, evidence-based telephone counselling service for smoking cessation. Quitline is tailored to meet the needs of priority populations including pregnant women, patients living with mental illness, and young people. Quitline also provides counsellors who are Aboriginal and/or Torres Strait Islander, and can assist people with hearing or speech impairment, or for those needing an interpreter.
Quitline counsellors are counselling professionals who use behaviour change techniques and motivational interviewing. Over multiple calls, Quitline counsellors use core counselling skills to help people plan, make and sustain a quit attempt.
There is evidence that making a proactive referral to Quitline, rather than simply recommending your patient to call, will result in a 13-fold increase in the proportion of patients using behavioural intervention in a quit attempt.
Make a referral to QuitlineSmoking cessation pharmacotherapies include nicotine replacement therapy (formulations include nicotine patch, gum, lozenge, mouth spray), varenicline and bupropion.
Varenicline and bupropion are not currently recommended in pregnancy due to limited efficacy and safety data.
Nicotine replacement therapy (NRT) may be used in pregnant women, noting that:
- Non-pharmacological interventions such as multi-session behavioural intervention (for example Quitline) are recommended as first-line therapy.
- NRT in conjunction with behavioural intervention may be considered in women unable to achieve abstinence using non-pharmacological interventions alone, or those with moderate to high nicotine dependence. Patients are more likely to stop smoking when pharmacotherapy is combined with behavioural intervention (Quitline).
- The risks and benefits of NRT should be discussed with the patient prior to initiation.
- NRT should be used at the lowest effective dose for the shortest duration possible.
Nicotine Replacement Therapy (NRT) and pregnancy
NRT is effective for increasing smoking cessation during pregnancy.
Formulations include:
- Transdermal – nicotine patch
- Faster-acting – nicotine gum, lozenge, and mouth spray.
Combination NRT therapy uses a nicotine patch together with a faster-acting formulation.
Pregnant women who have relapsed in the past or who experience cravings using one formulation of NRT alone, may use combination therapy under medical supervision.
Nicotine mouth spray contains a small amount of alcohol and is not considered first-line therapy in pregnancy.
If a nicotine patch is used, it should be removed at bedtime to minimise adverse effects and fetal exposure to nicotine.
Nicotine patches are currently subsidised by the Pharmaceutical Benefits Scheme (PBS). All formulations of NRT can be accessed over the counter through pharmacies and supermarkets.
NRT and breastfeeding
There is limited information available describing the use of NRT during breastfeeding. Maternal use of NRT is considered a safer option than continued smoking, and initiation of NRT is not a reason to stop breastfeeding.
As with during pregnancy, it is generally recommended that women attempt to stop smoking using non-pharmacological interventions alone in the first instance.
If indicated, NRT should be used at the lowest effective dose for the shortest duration possible to minimise the breastfed infant's exposure to nicotine.
The faster-acting NRT formulations have the flexibility for timing of use around breastfeeding. Allowing approximately 2 to 3 hours before resuming breastfeeding can help to reduce nicotine exposure in the breastfed infant.
Learn more in the Supporting smoking cessation in pregnancy and breastfeeding guideline (PDF), (general practice and health services versions) developed by Quit in collaboration with The Royal Women’s Hospital Pharmacy Department.
There are currently no TGA-approved vapes registered in the Australian Register of Therapeutic Goods (ARTG). This means that vapes have not been assessed by the TGA for safety, quality and efficacy, and their long-term health impacts remain unknown.
Vapes are not recommended by the RACGP or the Royal Women's Hospital's and Quit's clinical guidelines in pregnancy, due to limited efficacy and safety data.
Vaping cessation
Smoking during pregnancy is a well-established cause of adverse perinatal outcomes, and emerging evidence shows this may be the case with the use of vapes as well. There is limited research on interventions specifically targeting vaping cessation in pregnancy. If possible, pregnant women should be encouraged to quit vaping using behavioural support. If quit attempts are unsuccessful, faster-acting buccal forms of NRT may be considered. Varenicline and bupropion are not recommended due to limited efficacy and safety data.
Clinically significant drug interactions occur with tobacco smoke.
This Drug interactions with smoking (PDF) table lists medications and drugs that may require dosage adjustments when smoking is stopped. Patients should be regularly monitored with regard to their smoking status and doses of relevant drugs adjusted accordingly.
Visit the Clinical Tools & Guidelines page for:
- RACGP Clinical Guidelines (PDF)
- Smoking and pregnancy factsheet (PDF)
- Supporting smoking cessation in pregnancy and breastfeeding - General Practice (PDF).
Visit the Events page for:
- Upcoming events such as conferences, webinars and podcasts
- Past events including recorded webinars and podcasts such as the Australian Prescriber podcast: Therapeutic vapes for smoking cessation and nicotine dependence
Visit the Online Training page for:
- Quit online training modules for maternity care professionals on smoking cessation
Visit the Latest News & Research page for:
- News and announcements
- Relevant research in smoking and vaping cessation
- Quit Centre Quarterly newsletters.
Additional resources:
Visit Facts & Issues: Tobacco in Australia. A comprehensive review of the major issues on smoking and health in Australia, compiled by Cancer Council Victoria.
Australian Institute of Health and Welfare. Australia's mothers and babies [Internet]. Canberra: Australian Institute of Health and Welfare, 2025 [cited 2025 Sep. 9]. Available from: https://www.aihw.gov.au/reports/mothers-babies/australias-mothers-babies
Australian Institute of Health and Welfare. National Core Maternity Indicators [Internet]. Canberra: Australian Institute of Health and Welfare, 2024 [cited 2025 Sep. 9]. Available from: https://www.aihw.gov.au/reports/mothers-babies/national-core-maternity-indicators
Chamberlain C, O’Mara-Eves A, Porter J, Coleman T, Perlen SM, Thomas J, McKenzie JE. Psychosocial interventions for supporting women to stop smoking in pregnancy. Cochrane Database Syst Rev. 2017 Feb 14;2(2):CD001055. Available from:
https://pubmed.ncbi.nlm.nih.gov/28196405/
Claire R, Chamberlain C, Davey MA, Cooper SE, Berlin I, et al. Pharmacological interventions for promoting smoking cessation during pregnancy. Cochrane Database of Systematic Reviews, 2020; 3:CD010078. Available from: https://www.ncbi.nlm.nih.gov/pubmed/32129504
Greenhalgh, EM, Ford, C and Winstanley, MH. 3.8 Child health and maternal smoking before and after birth. In Greenhalgh, EM, Scollo, MM and Winstanley, MH [editors]. Tobacco in Australia: Facts and issues. Melbourne: Cancer Council Victoria; 2021. Available from https://www.tobaccoinaustralia.org.au/chapter-3-health-effects/3-8-child-health-and-maternal-smoking
Greenhalgh, EM, Stillman, S and Ford, C. 7.1 Health and other benefits of quitting In Greenhalgh, EM, Scollo, MM and Winstanley, MH [editors]. Tobacco in Australia: Facts and issues. Melbourne: Cancer Council Victoria; 2020. Available from https://www.https://www.tobaccoinaustralia.org.au/chapter-7-cessation/7-1-health-and-other-benefits-of-quitting
Greenhalgh, EM, Ford, C and Winstanley, MH. 3.7 Pregnancy and smoking. In Greenhalgh, EM, Scollo, MM and Winstanley, MH [editors]. Tobacco in Australia: Facts and issues. Melbourne: Cancer Council Victoria; 2021. Available from https://www.tobaccoinaustralia.org.au/chapter-3-health-effects/3-7-pregnancy-and-smoking
Jenkins, S, Hanley-Jones, S, Ford, C and Greenhalgh, EM. 7.11 Smoking cessation and pregnancy. In Greenhalgh, EM, Scollo, MM and Winstanley, MH [editors]. Tobacco in Australia: Facts and issues. Melbourne: Cancer Council Victoria; 2025. Available from https://www.tobaccoinaustralia.org.au/chapter-7-cessation/7-11-smoking-cessation-and-pregnancy
Marshall H, Vandeleur M, Dean E, Barton C, Luxton N, Carson-Chahhoud K, et al. Thoracic Society of Australia and New Zealand (TSANZ) Guidance for the Management of Electronic Cigarette Use (Vaping) in Adolescents and Adults. Respirology. 2025;30(7):605-22. https://doi.org/10.1111/resp.70066
Quit. Supporting smoking cessation in pregnancy and breastfeeding – Guideline. Version 2.0 May 2024. Available from: https://www.quitcentre.org.au/clinical-tools/type:guideline
Shobeiri F and Jenabi E. Smoking and placenta previa: a meta[1]analysis. Journal of Maternal-Fetal and Neonatal Medicine, 2017; 30(24):2985-90. Available from: https://www.ncbi.nlm.nih.gov/pubmed/27936997
US Department of Health and Human Services. How tobacco smoke causes disease: the biology and behavioral basis for smoking attributable disease. A report of the US Surgeon General, Atlanta, Georgia: US Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, 2010. Available from: https://www.ncbi.nlm.nih.gov/books/NBK53017/
US Department of Health and Human Services. The Health Consequences of Smoking: 50 Years of Progress. A Report of the Surgeon General. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, 2014. Available from: http://ncbi.nlm.nih.gov/books/NBK179276/pdf/Bookshelf_NBK179276.pdf.
The Royal Australian College of General Practitioners. Supporting smoking & vaping cessation: A guide for health professionals https://www.racgp.org.au/getmedia/924ba55d-dc47-41f9-bf5b-7a4cf9e19963/RACGP-NVP-and-Vaping-Cessation-September-2024.pdf.aspx, accessed 1 April 2025.
Vidrine JI, et al. Ask-Advise-Connect: A new approach to smoking treatment delivery in health care settings. JAMA Intern Med. 2013;173(6):458–64. Available from: https://pubmed.ncbi.nlm.nih.gov/23440173/
Wilson, HK, Zwar, N. Assisting young people aged 12-25 years to cease e-cigarette use in general practice. Aust J Gen Pract. 2024 May; 53(5):311-316. RACGP - Assisting young people aged 12-25 years to cease e-cigarette use in general practice
Winnall, W, Greenhalgh, EM and Scollo, MM. 18.6.1 Health effects of e-cigarette use during pregnancy. In Greenhalgh, EM, Scollo, MM and Winstanley, MH [editors]. Tobacco in Australia: Facts and issues. Melbourne: Cancer Council Victoria; 2023. Available from: https://www.tobaccoinaustralia.org.au/chapter-18-e-cigarettes/18-6-the-health-effects-of-e-cigarette-use/18-6-1-health-effects-of-e-cigarette-use-during-pregnancy
Last updated: 24 September 2025
